From social responsibility to medical innovation
Behind our charity is a vision of social and medical innovation derived from a strong sense of responsibility for the patient.
Before London’s Air Ambulance, seriously injured patients were dying unnecessarily because of the delay in receiving prompt and appropriate medical care.
The doctor on board model for air ambulances, which we pioneered, aims for effective delivery of time critical interventions when the patient needs them rather than when the healthcare system can comfortably provide them.
London's Air Ambulance was established in 1989 in response to a report by The Royal College of Surgeons, which documented unnecessary deaths from trauma and criticised the care that seriously injured patients received in the UK.
Scroll through our history...
-

Apr 2026
After 24 years of delivering the ground-breaking Physician Response Unit (PRU), the service moved to be under the management of the NHS, marking a huge achievement for both the charity and PRU.
-

Nov 2025
We launched a new resource – ‘When someone I love is in hospital’ – a workbook created and designed to be a tool for parents and caregivers to start a conversation with their child/children when someone they love is in hospital.
-

Nov 2025
We announced the appointment of Dr Anne Weaver as our new Medical Director. Anne takes over from Dr Tom Hurst, who has held the post since 2019.
-

May 2025
For the first time ever in the UK, we brought ECMO to the streets of London, offering hope to patients in cardiac arrest.
-

Mar 2025
We launched our new organisational strategy, which will see us through to 2039, our 50th year of operation.
-

Nov 2024
We announced Stef Reid as a new celebrity ambassador for London’s Air Ambulance Charity as she pledged her support to our vital service.
-

Oct 2024
We welcomed our two new Airbus H135 helicopters into service, with the company of HRH Prince William and David Beckham.
-

Aug 2024
We announced that our partnership with Omaze – which launched in June 2024 – raised £4 million. This incredible result meant we surpassed our appeal target of £15 million to replace our two helicopters and keep them flying for years to come.
-

Aug 2024
We announced that the £15 million target needed to replace our two helicopters was met ahead of schedule. Thanks to incredible support from the people, businesses and communities of London, we raised an amazing £16 million to replace our two helicopters and keep them flying for years to come, continuing to save lives across London every day.
-

Jun 2024
We were chosen by Omaze to be its charity partner and therefore recipient of funds raised by their next house draw: securing the incredible minimum figure of £1 million for our Up Against Time appeal.
Read more about the partnership and see the house available to win here.
-

Feb 2024
Our Black and White Gala, attended by HRH Prince William, Tom Cruise and other VIPs, raised an outstanding £1.3 million, surpassing all our previous galas.
-

Nov 2023
Philanthropists Julia and Hans Rausing supported our Up Against Time appeal with a seven-figure donation.
-

Oct 2023
We replaced our current rapid response car fleet with six new hybrid Volvo XC90s.
-

Sep 2023
London’s Air Ambulance Charity launched a one-of-its-kind booklet – 12 memories of sudden and unexpected loss – in which 12 families came together with their most pertinent and treasured memories of losing a loved one.
-

Aug 2023
London’s Air Ambulance Charity was once again featured in Channel 4’s documentary, Emergency.
-

Aug 2023
Throughout Friday 4 August, BBC London provided the charity with unprecedented coverage through a live news broadcast from our helipad, atop The Royal London Hospital in Whitechapel.
-

May 2023
Innovation Circle Member created London’s Air Ambulance’s first-ever Helipad Wellbeing Fund.
-

Mar 2023
London’s Air Ambulance Charity's Physician Response Unit (PRU) announced Sophie Mitchinson as the new Clinical Lead.
-

Mar 2023
The London Freemasons pledged £3 million towards the Up Against Time appeal; the largest single donation of the charity’s helicopter fundraising appeal.
-

Dec 2022
Gaby Roslin – an English TV and radio presenter – became a celebrity ambassador for London’s Air Ambulance Charity and pledged her support for our Up Against Time appeal.
-
Dec 2022
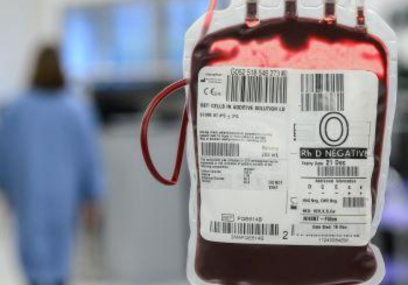
London’s Air Ambulance Charity spearheaded an innovative whole blood trial, SWIFT, testing air ambulances across the country carrying ‘whole blood’ instead of separate red blood cells and plasma.
-

Oct 2022
The Physician Response Unit (PRU) wing of our service launched its third team. As a result, the geographical footprint of the PRU expanded to cover Barking, Havering and Redbridge, alongside the existing operations in Tower Hamlets, Newham and Waltham Forest.
-

Oct 2022
We launched the biggest appeal in the charity's history - the Up Against Time appeal. The appeal must raise £15 million by 2024 to replace our helicopter fleet, as the current helicopters come to the end of their lifespan.
-

May 2022
We officially opened London’s Air Ambulance’s new helipad space, which will shave seconds off the advanced trauma teams’ response times and improve crew wellbeing.
-

May 2022
The Board of Trustees' diversity is improved with the appointment of five new trustees: Rita Chadha, Bianca Gill, Sheri Adigun, Gordon Pitman and Nick Goodwyn.
-

Apr 2022
We hosted our most successful gala to date, raising over £1,020,000 in donations.
-

Feb 2022
The Board of London's Air Ambulance Charity announced the appointment of Bob Forsyth as the new Chair of the Board of Trustees.
-

Jan 2022
PRU celebrated 20 years of operation after it was launched in 2002 with the aim to deliver safe, effective and patient-centric emergency care by bringing the Emergency Department to the community.
-

Dec 2021
The first-ever Royal Naval Nurse joined the Physician Response Unit (PRU) team.
-

Dec 2021
Third trauma team “Medic 3” was launched, allowing the service to reach even more patients and potentially save hundreds more lives.
-

Jun 2021
Sadiq Khan, the Mayor of London at the time, pledged support for London’s Air Ambulance Charity.
-

Apr 2020
A second PRU team was launched.
-

Jan 2019
London’s Air Ambulance Charity marked its 30th anniversary and announced HRH The Duke of Cambridge as royal patron of its campaign. As a former air ambulance pilot, His Royal Highness Prince William championed those working on the frontline and highlighted the importance of our rapid response and cutting-edge medical care.
-

Oct 2018
London's Air Ambulance Charity launched a landmark new study in an aim to reduce deaths due to catastrophic bleeding, thanks to funding from Barts Charity, Saracens and The Henry Surtees Foundation.
-

Oct 2017
Working with Barts Health NHS trust, we began the delivery of a new clinical model to work towards a consultant-led service. A consultant is now present on most clinical missions alongside the duty crew including a doctor and a paramedic, ensuring that patients have the best possible care.
-

Aug 2017
The remodelled PRU was launched thanks to funding from Tower Hamlets Together. Previously an eight-hours-a-day, five-days-a-week service, the PRU now responds to 999 calls 12 hours a day, seven days a week, all year round.
-

Nov 2016
London's Air Ambulance Charity won the Emergency Services category at the Daily Mirror Pride of Britain Awards. The medical team who worked on 24-year-old cyclist Victoria won the award for its use of REBOA (Resuscitative Endovascular Balloon Occlusion of the Aorta) - to prevent her from bleeding to death at the roadside.
-

Jan 2016
Following the ‘Your London, Your Helicopter’ campaign, London’s Air Ambulance’s second helicopter was launched and operational in London.
-

Mar 2015
For the first time in its history, London’s Air Ambulance flew longer hours during summer. From 29 March 2015, the start of BST, until 2 September, the charity delivered its advanced trauma team to critically injured people in London via helicopter every day until sunset.
-

Mar 2015
London Freemasons pledged £2 million for the second helicopter. London Freemasons launched an appeal to its 40,000 members across 1,350 lodges in London to fundraise towards the £2 million target.
-

Feb 2015
The ‘Your London, Your Helicopter’ campaign was launched to raise the funds for a second helicopter.
-

Feb 2015
A life-saving dispatch app was launched with EE, helping London’s Air Ambulance save lives by reducing the time it takes to dispatch the charity’s advanced trauma teams by up to two minutes.
-

Jan 2015
The first Paramedic Education and Development Lead at Barts Health NHS Trust was appointed to work with London's Air Ambulance. Graham Chalk took up the role following 11 years as a Lead Paramedic and Clinical Liaison Officer.
-
Jun 2014
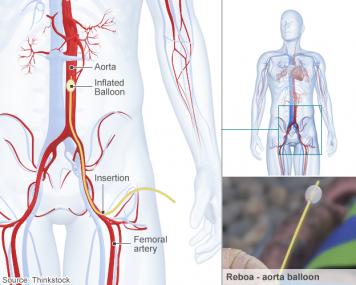
The world’s first pre-hospital REBOA (Resuscitative Endovascular Balloon Occlusion of the Aorta) was performed. This balloon surgery is used to control severe pelvic bleeding, an injury most commonly associated with cycling incidents and falls from height.
-

May 2014
The rapid response cars received a new look. Bringing uniformity to London’s Air Ambulance fleet, the ŠKODA Octavia vRS Estate vehicles sported the same red livery as the helicopter and were emblazoned with the high visibility Battenberg strips required on emergency vehicles.
-

Mar 2014
The Chancellor of the Exchequer announced that London’s Air Ambulance Charity was to receive £1 million to enable the charity to operate a second helicopter.
Image: Photo credit - BBC
-

Mar 2014
Their Royal Highnesses The Earl and Countess of Wessex visited London’s Air Ambulance Charity as part of a tour of two charities supported by the Wessex Youth Trust on the Earl’s 50th birthday. TRH The Earl and Countess of Wessex awarded London’s Air Ambulance Charity a grant for over £10,000.
-

Feb 2014
UK's first Patient Liaison Nurse for trauma patients was appointed, funded by the City of London Corporation's charity, City Bridge Trust.
-

Feb 2014
The Institute of Pre-Hospital Care at London’s Air Ambulance Charity partnered with Barts and the London School of Medicine at Queen Mary University of London to create the UK’s first Intercalated BSc degree in Pre-Hospital Medicine.
Image: The Institute of Pre-Hospital Care’s logo at the time
-

Aug 2013
Boris Johnson, Mayor of London at the time, visited the helipad. “I am very proud that London’s Air Ambulance has such a world-leading reputation for delivering the most cutting edge advanced trauma care outside of hospital - care that is saving countless lives. That has only been possible because of the generosity of Londoners to date,” he said.
-

Feb 2013
The aircraft overnight base moved from Denham to the Royal Air Force base in South Ruislip, Northolt. The relocation reduces flight time to and from the helipad at The Royal London Hospital in Whitechapel, thereby saving on fuel costs.
-

Feb 2013
The helicopter received new livery: the red helicopter is emblazoned with emergency markings and the charity’s key messages to create greater awareness of London’s Air Ambulance Charity’s work and the need for support.
-

Sep 2012
Sir Stirling Moss thanked London's Air Ambulance Charity after he suffered a terrible fall in his home in 2010. Within minutes, our specialist doctor and paramedic trauma team was at his side providing advanced medical care.
-

Mar 2012
London's Air Ambulance was the first air ambulance in the UK to carry blood on board. The initiative, lead by Dr Anne Weaver, brought blood transfusion to the roadside.
-

Dec 2011
The service moved to a new helipad at the top of The Royal London Hospital, 17 floors above Whitechapel Road. At 284ft, the helipad is the highest in Europe and is almost the same height as Big Ben.
-

Aug 2011
The first pre-hospital emergency medicine professor in the UK was appointed.
Image: Prof. David Lockey.
-

Jan 2010
London's Air Ambulance secured the funding to serve London around the clock, using rapid response cars throughout the night when it's too dangerous to land in London. This would not have been possible without the London Ambulance Service's decision to fund the wages of all paramedics.
-

Nov 2007
The Pre-Hospital Care Programme was established in collaboration with Barts, the London School of Medicine and the London Ambulance Service. The first of its kind in the UK, it offered a chance for selected students to become part of a structured programme, allowing them early clinical exposure to the pre-hospital environment.
-

May 2006
The first-ever London Trauma Conference occurred, meaning London became home to one of the most prestigious trauma education and research events in the world, led by Dr Gareth Davies and Prof David Lockey.
-

Jan 2006
London's Air Ambulance Charity's lottery was launched. Contributing £1 a week now gives supporters a chance to win £1,000 while providing the charity with a regular income.
Image: Lucky lottery winners Lynda Stevens and her husband Ron receive their prize at the helipad
-

Jul 2005
The Mayor of London, Ken Livingstone, visited London's Air Ambulance Charity in the aftermath of 7 July 2005 bombings.
Image: Ken Livingstone during his visit with Dr Gareth Davies, Medical Director at London's Air Ambulance
-

Jul 2005
A royal visit in recognition of London's Air Ambulance's contribution during the capital's emergency medical response to the 7 July 2005 bombings took place shortly after the incident.
Image: HM the Queen at London's Air Ambulance Charity.
-

Jul 2005
On 7 July 2005, London’s Air Ambulance dispatched 18 medical teams to the sites of the London bombings, helping to triage and treat over 700 patients. Sadly 52 people were killed in the series of coordinated terrorist attacks in central London, which targeted civilians using the public transport system during the morning rush hour.
-

Jan 2004
London's Air Ambulance Charity gained recognition abroad for its governance, patient care standards and life-saving innovation. It is now a world-leading institution.
Image: Japanese translation of The Study of Helicopter Emergency Medical Services in London
-

May 2002
Potters Bar Train Crash - 10 May 2002
Seven people were killed and 70 injured when a train derailed in Hertfordshire. London’s Air Ambulance delivered advanced trauma teams to the scene of the incident and helped coordinate the emergency medical response, working alongside the London Ambulance Service.
-

Jan 2001
The Physician Response Unit (PRU) was launched. Operated by London's Air Ambulance, the PRU responds to medical emergencies, such as cardiac arrests. It operates in the area around The Royal London Hospital, including the City and East London. Now expanded, but with the same focus of getting care to the patient where they need it, it continues to serve the local community to the present day.
-

Jan 2000
The first Driver Standards Manager was appointed. Paul Smith was made responsible for managing our fleet of rapid response cars and training our paramedics to drive on blue lights through night-time London quickly and safely.
-

Oct 1999
Paddington Train Crash - 5 October 1999
Two trains collided, sadly resulting in 31 deaths and over 220 people being injured. London’s Air Ambulance delivered four advanced trauma teams to the site and helped coordinate the emergency medical response, alongside the London Ambulance Service.
-

Mar 1999
The first rapid response car was introduced and the service expanded into night-time operations. London’s Air Ambulance starts delivering the same medical team and equipment to critically injured people after dusk by road. Initially limited to four nights a week, the night-time operations gradually expanded until the charity started operating 24/7 in 2010.
-

Feb 1999
At an improvised stall carried around by Christine Margetts, Medical Secretary to Dr Gareth Davies, umbrellas and baseball caps were available to purchase, with all proceeds going to London’s Air Ambulance Charity. This was the birth of the charity as we know it and Christine continued to work for the charity for the next 20 years.
-

Jan 1999
London’s Air Ambulance Charity and Virgin called for support from the public, in particular the business community of London. “I go back to the benefit to a commercial company of spending some of its profits on a very worthwhile and very public operation. For companies, this is tax deductible stuff,” said Andrew Cameron, Chief Executive of London's Air Ambulance.
-

Jan 1998
The service attained a new helicopter: the Dauphin is replaced by MD902 Explorer. This model was chosen for its safety features, which include no tail rotor (important in an urban environment).
-

Dec 1997
Virgin got on board. “I realised it was time to pay back,” said Richard Branson, revealing in a press release that he had been rescued by emergency helicopters five times. London’s Air Ambulance now had the backing of a powerful PR mogul as well as vital financial support from Virgin Group.
Virgin purchased the helicopter from the Daily Express and covered the operational costs.
Image: London's Air Ambulance helicopter livery reflects Virgin's sponsorship of the charity
-

Jan 1997
The media debate over proposed funding cuts, which would have shut down London’s Air Ambulance, stirred emotion. The public, once again, voiced their concerns and showed their support for the service.
-

Dec 1996
Sceptics of the service continued to challenge the model of pre-hospital care pioneered by London's Air Ambulance. The result was a further review by Deloitte. The review considered several alternative options, including confining helicopter operations to outer London or replacing it completely with several specialist road ambulances.
-

Dec 1996
Patients and the public came to the rescue. A media battle ensued after medical professionals voiced criticism in the national media, with some of the patients saved by London’s Air Ambulance approaching journalists to tell their stories.
-

1996
Although trauma networks and trauma systems didn't exist (yet), The Royal London Hospital was functioning as a major trauma centre. Today, the hospital is the UK's leading major trauma centre.
-

1996
Dr Gareth Davies became Medical Director of London's Air Ambulance. In the same year, Prof Tim Coats became a consultant for the service. Tim was the first senior lecturer in A&E and pre-hospital care in the UK.
Image: Dr Gareth Davies (photo 2015) and Prof Tim Coats
-

Jul 1994
A report commissioned by the Department of Health, colloquially known as the Sheffield Report, is published. Designed to evaluate the efficiency of London’s Air Ambulance and its model of pre-hospital care, the report's conclusions are likely to influence funding decisions.
-

1994
Another change to the livery: the helicopter was painted yellow.
Image: The helicopter in Daily Express livery.
-

Dec 1993
London’s Air Ambulance performed the world’s first successful open heart surgery at the roadside. This pioneering procedure challenged the guidelines on resuscitation as a self-fulfilling prophecy. The non-conventional approach and personal courage of individual doctors pushed the boundaries of pre-hospital care and continues to save lives today.
-

Apr 1993
Bishopsgate Bombing - 24 April 1993
One person is killed and 44 injured when the IRA detonate a truck bomb in the City of London. That day, London’s Air Ambulance was being followed by a filming crew from the ITV documentary series Blues and Twos and the charity’s response was captured on camera.
-

Mar 1993
In March 1993, the 'White Dauphin' changed livery to orange.
-

1992
First Lead Paramedic and Clinical Liaison Officer were appointed. Charlie Balderstone took up the role, acting as the main point of contact between London's Air Ambulance and the London Ambulance Service.
Image: Charlie Balderston
-

Jan 1991
Cannon Street Station Train Crash - 8 January 1991
London’s Air Ambulance landed on the tracks just yards behind the train, bringing five medical teams to the site. The team helped to coordinate the emergency medical response to the incident, working alongside the London Ambulance Service.
-

Nov 1990
London’s Air Ambulance was branded a “disaster for the local people” in a London newspaper. Labour Councillor John Biggs was quoted to have said: “The helicopter takes off and lands with a deafening noise drowning conversation and disturbing the peace of people in the area.”
-
1990
The first flight from Biggin Hill occurred: a small airport in South East London which served as an initial base for London’s Air Ambulance. To this day, our helicopter refuels at this airport.
Image: Graphics by bigginhillairport.com
-
Jan 1990
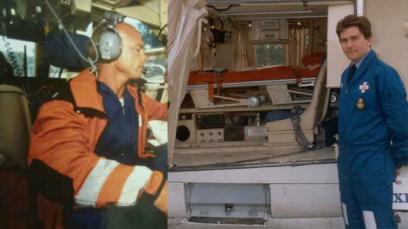
The first doctor and paramedic were introduced on board. The first paramedics to do the job were Chris Mayer and Tony Crann, who started as part of a group of 10 selected by the London Ambulance Service from all over London. The first senior clinician to accompany a paramedic on board was Dr Mark Dalton, known in the hospital corridors as Bald Eagle One.
Image: Dr Mark Dalton and Tony Crann
-

Sep 1989
Our first mission was completed: the helicopter flew organs for a transplant from Scotland to London. Since then, the purpose of the service has changed drastically; the charity now delivers an advanced trauma team to the roadside.
Image: The transplant team was picked up at the Royal Free Hospital and flown to Dundee
-

Jan 1989
London’s Air Ambulance Charity is set up as a joint initiative between:
• Daily Express - Andrew Cameron and Lord Stevens
• The Royal London Hospital - Richard Earlam and Alastair Wilson
• NHS - Conservative Government led by Margaret Thatcher.Image: London’s Air Ambulance’s first logo.
-

1989
London Ambulance Service got on board in support of London's Air Ambulance. To this day, the London Ambulance Service provides paid paramedics who work with London's Air Ambulance.
-

Dec 1988
The first helicopter, call sign G-HEMS, is flown into Trinity Square Gardens, London.
-

Nov 1988
The Royal College of Surgeons of England issued a report documenting cases of patients dying unnecessarily because of the delay in appropriate medical care.
-

1988
Express Newspapers agreed to provide London's Air Ambulance with a helicopter, pilots, operational staff and all running costs for four years – approximately £4 million.
Image: Letter from Lord Stevens of Ludgate, Chairman of United Newspapers plc., published in Trauma Care by R. Earlam; 1997.
-

Apr 1986
London’s Air Ambulance was just a vision and aspiration of clinicians at The Royal London Hospital, who clearly articulated the need for a helicopter emergency medical service.
-

1986
London’s Air Ambulance came to life through a casual conversation. The basis was laid on the tennis court where the wives of Richard Earlam, Consultant Surgeon at The Royal London Hospital, and Lord Stevens of Ludgate, Chairman of United Newspapers plc., discussed trauma care in Germany.
-
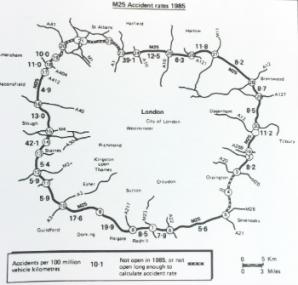
1985
Rapidly increasing traffic levels in London coupled with road traffic collision statistics illustrate the urgent need for a helicopter emergency medical service.
Image: M25 accident rates, 1985 map

